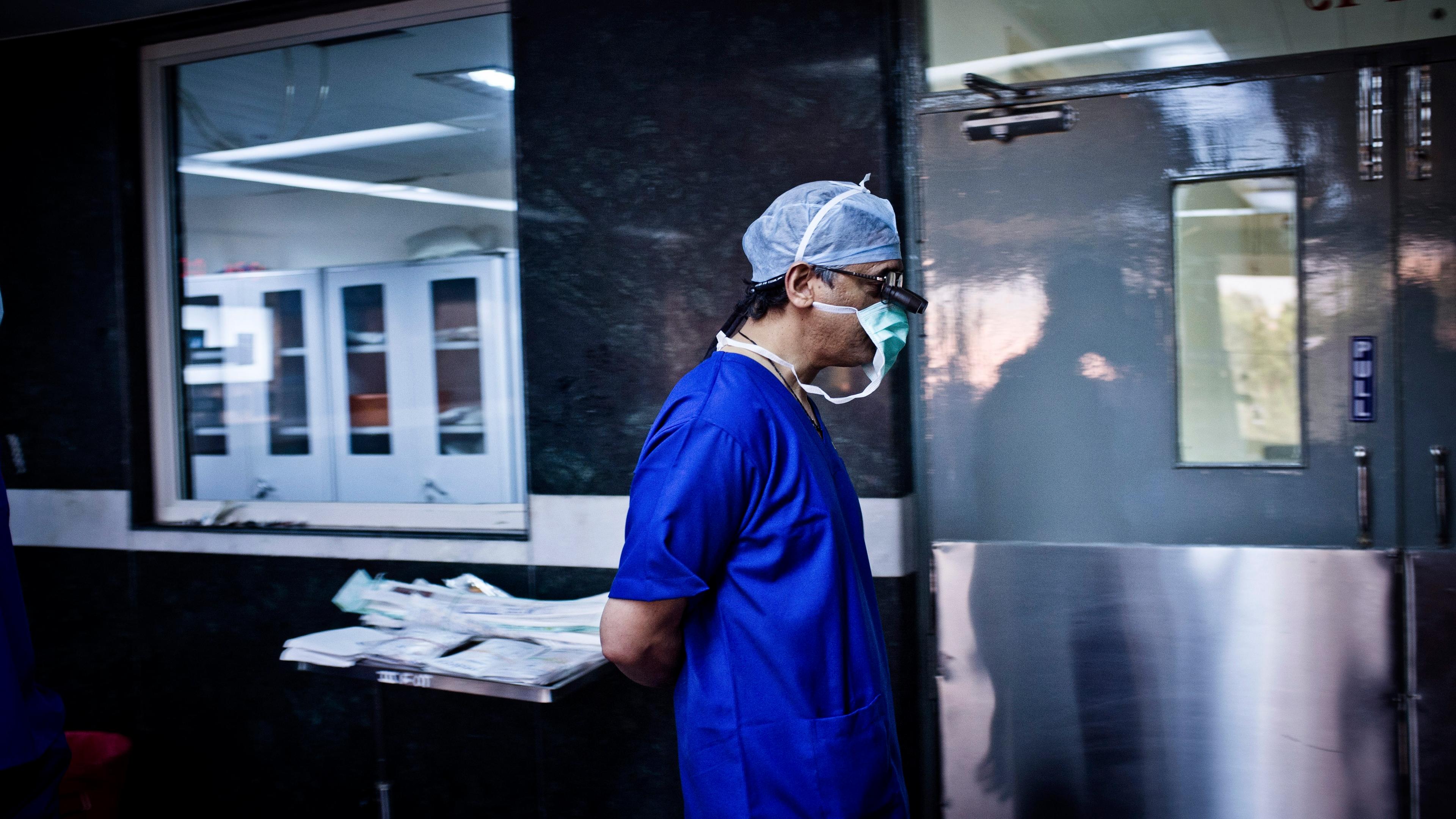
‘Dr Glaucomflecken’ has nearly 600,000 followers on Twitter and 1.7 million on TikTok. He’s an ophthalmologist in the United States (real name Will Flanary), and a comedian, and he spends his time making short clips stereotyping different healthcare specialities and their supposed personality traits. In one of his videos, a general surgeon meets his new medical student. The surgeon is predictably gruff and emotionally distant, barking orders, squashing enthusiasm, and instructing the student to undertake menial tasks.
In making these videos, Dr Glaucomflecken is drawing on a long and fraught history of healthcare professionals’ idealised or stereotyped personality traits and emotional tendencies. And in these stereotypes, surgeons possess some of the most obvious and culturally salient characteristics. Mostly male, authoritarian and paternalistic, the worst version of the stereotypical surgeon is volatile, insistent, even abusive – and prone to unpredictable outbursts of anger. He cuts first, asks questions later, and is never in doubt. He is good at ‘hard’ surgeries but bad at ‘soft’ skills, like compassion and communication. Academically or technically brilliant, he lacks emotional intelligence. He operates with dispassion, but occasionally his capacity for emotional detachment tips into cruelty – causing psychological harm to both himself and his patients. He is often white and, at the very least, upper middle class.
No one embodies this caricature better than Richard Gordon’s irascible Sir Lancelot Spratt. Spratt first appeared in Gordon’s novel, Doctor in the House (1952). The film adaptation by the same name was released in 1954, and starred Dirk Bogarde as a young medical student, and James Robertson Justice as the fearsome surgeon Spratt. A dictatorial demagogue, Spratt strode down hospital corridors with a gaggle of frightened trainees hurrying along behind him. In one iconic scene from the film, Spratt stands at a patient’s bedside firing questions at a group of medical students, one of whom has just examined the hapless and prone sufferer and found a lump. ‘Is it kidney? Is it spleen? … Is it dangerous?’ barks Spratt, before drawing a long incision line on the patient’s abdomen, then turning to the by now highly alarmed patient to say: ‘Now don’t worry, this is nothing whatever to do with you.’
By the time Gordon’s first Doctor novel was published (the popular series grew to 18 titles), the stereotypes Spratt personified were already five decades old. While in the early 19th century, surgeons were relatively emotionally expressive, by the dawn of the 20th, the cultures of medicine and society had changed. The introduction of things like anaesthesia and antisepsis meant that surgery specifically became much more effective. Surgeons no longer had to rely on their personalities to attract patients – they could cure them instead. The end of Queen Victoria’s reign also saw the development of more stoic forms of medical masculinity. Outpourings of feeling became less acceptable and, as cultural historians like Michael Brown have shown, the healing professions became more focused on their contributions to the national good, and less on the emotional dimensions of individual patient care.
As both Gordon’s and Dr Glaucomflecken’s success demonstrates, these characteristics endured through the 1950s and into the present. While some aspects are unpleasant, and vulnerable to satire and critique, others – even the ones Gordon mocks – are held up as positive elements of the surgical personality. Quick decision-making, the ability to exert authority over both patients and colleagues, and emotional discipline or self-management are all still seen by many as crucial characteristics, essential to the making of a good surgeon. In the age of industrialised medicine, when surgery is a routine, almost mechanised practice, a certain degree of inhumanity is seen as advantageous. For example, for much of the 20th century, value has been placed on emotional detachment because of the idea that feelings could interfere with a surgeon’s ability to effectively and efficiently carry out their work.
These notions are held by people external to the profession – fiction-writers, TikTok-creators, television-producers, healthcare policymakers – and by surgeons themselves. Historians of emotion call this an ‘emotional regime’. This is the dominant mode of emotional expression and thought in different places and eras – the unspoken codes of emotional conduct.
In the past, these codes of conduct were upheld, and the surgical character was assessed, by social and professional peers, as well as by senior colleagues. In the middle decades of the 20th century, jobs were acquired via obvious and ostentatious nepotism, potential trainees were interviewed, and careers were made for men who were a ‘good fit’ with the culture of this or that hospital. More recently, standardised tests, letters of recommendation, and interviews have provided the basis on which applicants are selected.
But increasingly, medical educators, policymakers and some surgeons themselves are advocating personality testing as a method to identify people best suited to the profession and to weed out those who might prove unable to cope with the demands of the job.
One of the problems of current surgical selection and training is that it doesn’t seem, at first glance anyway, to be very successful. In the US, the national attrition rate of general surgical residents sits at approximately 20 per cent per year – higher than any other speciality. Which means that one in five of those who start out as surgeons leave for other specialities, or exit the medical profession entirely. Could this statistic be improved by making better decisions from the very beginning? And could a standardised, ‘objective’ personality test eliminate the kind of inequity, nepotism and bias (conscious and unconscious) that continues to permeate the surgical profession today?
The desire to identify the best-fit applicants is not unique to surgery; other high-stress careers such as aviation have studied the use of personality tests in applicant selection. And there have been plenty of studies focused on identifying the characteristics or emotional traits associated with currently practising or senior surgeons. However, it is only in the past few years that surgeons and medical educators have sought to use these tests to assess applicants.
First developed in the 1920s, the most famous personality test is perhaps the Myers-Briggs Type Indicator, which assigns people four categories: introversion or extraversion; sensing or intuition; thinking or feeling; and judging or perceiving. In 2013, the personality assessment industry in the US was estimated to be worth between $2 and $4 billion a year.
Myers-Briggs has pretty shaky evidentiary foundations, but other personality tests are more robust. For example, The Big Five, developed in the 1980s, groups personality traits into (yes, you guessed it) five: extraversion; agreeableness; conscientiousness; emotional stability (sometimes termed neuroticism and scored negatively); and openness. The Big Five test has been used in all sorts of industries, and various traits are associated with professional or academic achievement. A 2018 study applied the Big Five to surgical residents. Current trainees at the University of Texas Medical Branch were classified as either ‘low performing’ or ‘non-low performing’, and these groups were then compared with their personality-test scores to see if there was any correlation between certain traits and surgical success.
This study found that non-low-performing residents (‘good’ surgeons) scored significantly higher on certain traits – extraversion, conscientiousness and emotional stability. As a result, and because traditional assessment metrics did not distinguish between high- and low-performing residents, they determined that the Big Five test could be a useful tool to help identify successful applicants to general surgery residency. Their research found that ‘good’ surgeons were more likely to be assertive, energetic, outgoing, efficient, organised and thorough, and less likely to be forgiving, generous, sympathetic, self-pitying or worrying. A similar study from the same year argued that their personality testing indicated the existence of a ‘distinct and consistent’ ‘physician personality’. And there were ‘solid and reproducible’ differences between surgeons and other medical professionals. Another study found personality testing to be ‘a useful addition’ to conventional methods of paediatric surgical-fellow selection.
Personality tests, especially the ones that are self-administered such as Myers-Briggs, have something of a bad reputation. At their worst, they do little more than apply a gloss of social science objectivity to a very old, very subjective and very cultural sense of the strengths and weaknesses of different traits or characteristics. And their application to surgical assessment and training risks reifying problematic tropes and stereotypes. There are limits to the usefulness of supposed correlations between traits and performance. Just because a connection is observed between assertiveness and professional achievement, say, does not necessarily establish that all assertive surgeons will thrive or that it is a necessary precondition of success. Incorporating personality testing into selection also hazards homogenising the surgical profession – do we really need a bunch of extraverts in every operating theatre?
The abundance of research on the surgical personality reveals quite how alluring the subject is. Much of it is conducted by surgeons themselves – people researching what makes them them or seeking to distinguish themselves from their colleagues or trying to elevate their own professional status or reputation. And much of this interest is well-intentioned and motivated by practical concerns around attrition rates and burnout.
Despite this, efforts to address retention rates that focus on personality-typing often fail to interrogate a fundamental question: what does success in surgery look like, and why do only people with certain personalities seem to thrive in surgical settings? While there may well be personalities that tend to do well in an environment that requires quick decision-making, effective collaboration and the ability to work under pressure, perhaps the problems of retention lie in surgical culture, not in the characteristics of individuals. Testing aspiring surgeons for their assertiveness, efficiency and energy because those are the characteristics of residents who seem to be best at weathering the brutal training regimes of medicine recapitulates the status quo. It heavily implies that the ideal ‘non-low performing’ surgeon is born, rather than made. And neglects to consider the extent to which the surgical ‘personality’ is a developmental consequence of surgical training itself, rather than something innate.
We know, too, that surgery is an insufficiently diverse profession. The relationships between personality tests like the Big Five and gender, culture, ethnicity and age are complex. Recent studies have not only found that the test does not apply to people living in low- and middle-income countries. Even in Western nations, its applicability to older adults is limited because the model was originally developed by studying university students. The Big Five reveals big differences in personality between the genders, but depending on whether you say you are ‘male’ or ‘female’, the same answers can produce different personality assessments.
As discussed, emotional self-discipline has long been a key attribute of the ideal surgeon – and the ideal surgeon has historically been male. While the Big Five determines that conscientiousness is a key marker for surgical success – and women are more likely to score highly on that trait – the other traits that correlate with retention (assertiveness, extraversion, and emotional stability) are traditionally male attributes. It is perhaps unsurprising that men who adhere to conventional standards of masculinity thrive in environments made with them in mind, and alongside their peers. Studies have shown that these cultural aspects continue to deter women from the speciality, and make it harder for them to remain in the profession.
As the history suggests, what makes a good surgeon is in constant flux. This is particularly true now, as more and more members of the profession recognise the harmful and restrictive nature of deterministic stereotypes, and acknowledge the importance of a more diverse and inclusive speciality. While personality tests might have a place in surgical modernisation and diversification, they must be part of a broad ecosystem of reforms that include better mentorship, more family-friendly workplaces, greater autonomy, consequences for sexual harassment, more humane working hours, and a radical reduction in individual and institutional racism. Instead of finding solutions to the attrition rate in the character traits of individual surgeons, answers might be sought in the working environments, cultures, and conventions of the surgical profession and its history.